In the rapidly evolving landscape of healthcare, the effective management of projects is of paramount importance. This holds especially true for healthcare organizations within the UK’s National Health Service (NHS).
As these institutions seek to improve patient care, optimize resources, and adapt to an ever-changing environment, project management becomes the key to success.
Tailored for project managers within UK healthcare organizations, this comprehensive guide explores the methodologies that drive successful projects, aiming to provide you with a roadmap for navigating the challenges and opportunities unique to healthcare project management in the UK.
We’ll also shed light on the digital tools and software solutions that empower project managers to orchestrate healthcare initiatives efficiently, with a special focus on PM3, an award-winning project management tool in use by many NHS organisations.
Healthcare project management is a specialized discipline that plays a pivotal role in the healthcare industry’s pursuit of providing high-quality patient care, improving operational efficiency, and adapting to the ever-evolving healthcare landscape.
It is the systematic and strategic approach to planning, organizing, and executing complex projects within healthcare organizations to achieve specific objectives and goals.
These objectives can encompass a broad spectrum of healthcare-related initiatives, ranging from introducing innovative medical treatments, upgrading information technology systems, to constructing and equipping new medical facilities.
At its core, healthcare project management is about bringing structure and order to complex, multifaceted endeavours within the healthcare sector.
Here are some key aspects that define healthcare project management:
Project definition and scope
Healthcare projects can be as diverse as launching a telemedicine program, implementing a new electronic health records (EHR) system, or designing a more efficient patient admission process.
In Healthcare, a project manager’s role is to define project scopes, objectives, and boundaries to ensure clarity and alignment among team members and stakeholders.
Resource allocation and management
Efficient allocation of resources, including human resources, budget, and time, is crucial in healthcare project management.
Project managers must carefully balance these resources to ensure projects remain on track and within budget constraints.
Risk assessment and mitigation
Healthcare projects often involve a degree of risk, whether it’s regulatory changes, clinical uncertainties, or unforeseen technological challenges.
Project managers need to conduct thorough risk assessments and develop strategies to mitigate these risks to ensure successful project delivery.
Stakeholder engagement
Effective communication and stakeholder management are paramount in healthcare project management.
Project managers must engage with various stakeholders, including healthcare providers, business administration professionals, patients, regulatory bodies, and vendors. Clear and transparent communication helps in gaining support, resolving issues, and keeping everyone informed.
Quality assurance
In healthcare, the quality of care and services is paramount.
Project managers are responsible for incorporating quality assurance measures into projects to guarantee that patient care standards are met or improved during and after project implementation.
Adherence to regulations
The healthcare industry is highly regulated, and projects must comply with various laws, standards, and guidelines.
Healthcare project managers are well-versed in navigating these regulations and ensuring project activities align with legal requirements.
Change management
Implementing changes in healthcare organizations can be met with resistance from staff or patients.
Project managers often collaborate with change management experts to help transition healthcare teams smoothly into new processes, technologies, or workflows.
Post-implementation evaluation
Even after a project is completed, healthcare project managers continue to monitor and evaluate its impact on patient care and organizational efficiency.
This helps in identifying areas for further improvement and ensuring that the project’s benefits are sustained over time.

Healthcare project management holds a pivotal role within the healthcare industry, and its significance cannot be overstated.
In a field where patient well-being, operational efficiency, and adaptability are paramount, effective project management ensures the achievement of crucial objectives.
Here, we look into the reasons why healthcare project management is indispensable:
Improved patient care
At the heart of healthcare is the fundamental goal of delivering exceptional patient care.
Healthcare project management is the driving force behind initiatives aimed at enhancing patient experiences and outcomes.
By meticulously planning and executing projects, healthcare organizations can implement innovative treatments, streamline care processes, and improve clinical practices, all of which contribute to better patient care.
Cost control
In an era marked by rising healthcare costs, efficient resource management is imperative.
Healthcare project managers are adept at meticulously allocating budgets, optimizing resource utilization, and adhering to timelines.
Through their expertise, they help lower costs, making healthcare services more affordable and accessible to a wider demographic.
Regulatory compliance
Navigating the labyrinth of healthcare regulations and standards is a formidable task.
Healthcare project managers serve as navigators, ensuring that projects remain in compliance with the myriad of regulations governing healthcare.
This includes adherence to clinical standards, data security regulations, and healthcare privacy laws.
Their expertise is invaluable in maintaining legal and ethical standards within the industry.
Enhanced efficiency
Operational efficiency is the lifeblood of healthcare organizations.
Projects aimed at optimizing processes, adopting innovative technologies, and streamlining workflows can result in significant efficiency gains.
Healthcare project managers play a pivotal role in conceptualizing, planning, and executing these projects, ultimately leading to more efficient healthcare delivery.
Technology implementation
The rapid evolution of technology is reshaping the healthcare landscape.
Implementing project management tools requires precise planning, change management and careful execution.
Healthcare project managers are at the forefront of adopting and integrating these technologies, ensuring a seamless transition that minimizes disruptions and maximizes benefits.
Risk mitigation
Healthcare projects often carry substantial risks, ranging from clinical uncertainties to unforeseen logistical challenges.
Healthcare project managers are adept at identifying potential risks and developing comprehensive mitigation strategies.
Their expertise minimizes project disruptions, safeguards patient safety, and protects the organization’s reputation.
For a guide about risk communication in project management, check out our article Communicate Risks Effectively – How to Visualise Risks by Project Stage.
Effective project management methodologies are the backbone of successful healthcare projects.
These methodologies provide a structured approach to planning, executing, and delivering healthcare initiatives while addressing the unique challenges and requirements of the healthcare sector.
In this chapter, we explore the top three methodologies used in healthcare project management: Waterfall, Agile, and Hybrid.
Overview
The Waterfall methodology is a linear, sequential approach to project management.
It divides a project into discrete phases, with each phase building upon the previous one.
Healthcare projects often involve strict regulatory requirements and well-defined processes, making Waterfall project management an attractive methodology for projects where predictability and documentation are critical.
Key characteristics
Pros
Cons
Would you like to find out more about the Waterfall methodology? Check out our in-depth guide Advantages of The Waterfall Methdology.
Overview
Agile project management is characterized by its iterative and flexible approach.
It emphasizes collaboration, customer feedback, and rapid adaptation to changing requirements.
Agile is particularly well-suited for healthcare projects that require continuous improvements, such as software development, clinical trials, and patient care process optimization.
Key characteristics
Pros
Cons
Overview
The Hybrid methodology combines elements of both Waterfall and Agile to provide a balanced approach.
It’s an excellent choice for healthcare projects that require a degree of predictability while accommodating changes and flexibility.
Hybrid methodologies allow organizations to structure projects with phases while incorporating iterative elements.
Key characteristics
Pros
Cons
In healthcare project management, the choice of methodology depends on the project’s specific needs, regulatory requirements, and organizational culture.
Healthcare project managers must carefully evaluate each methodology’s pros and cons to select the one that aligns best with their project objectives and constraints.
Ultimately, the chosen methodology plays a critical role in the success of healthcare initiatives and the delivery of quality patient care.

Implementing effective project management practices within a healthcare organization is essential for achieving successful outcomes, whether it involves improving patient care, upgrading infrastructure, or optimizing operational processes.
This chapter explores the steps to seamlessly integrate project management into your healthcare organization’s culture and workflow.
Step 1. Define clear objectives and goals
Begin by setting clear, measurable, and achievable objectives for integrating project management.
During the planning stage, make sure you identify what your organization aims to accomplish through this initiative, namely your project benefits.
Common goals may include improving project success rates, increasing efficiency, or enhancing collaboration among teams.
Step 2. Establish a Project Management Office (PMO)
A Project Management Office (PMO) serves as the central hub for project management activities.
Create a dedicated team or department responsible for overseeing project management standards, methodologies, and best practices across the organization.
The PMO should consist of experienced project managers, coordinators, and experts who can guide and support projects.
Step 3. Select appropriate project management methodologies
Choose project management methodologies that align with your organization’s goals and project types.
Depending on the nature of projects, consider using traditional Waterfall, Agile, or Hybrid methodologies.
Ensure that your team is well-versed in these methodologies and can apply them effectively.
Step 4. Invest in training and development
Effective project management requires skilled professionals, which is why it’s important to invest in training and development programs to enhance the project management skills of your team members.
Encourage your employees to get certifications in project management frameworks, such as those provided by the Project Management Institute (PMI): Certified Associate in Project Management (CAPM); Project Management Professional (PMP); Program Management Professional (PgMP).
Step 5. Develop standardized processes and templates
Standardized processes and templates streamline project management efforts.
Create project management templates, including project charters, timesheets, risk assessment forms, and communication plans.
These tools ensure consistency and efficiency in project execution.
Step 6. Foster a culture of collaboration
Collaboration is key to successful project management.
Encouraging a culture of open communication and teamwork within your organization will help cross-functional teams to work together seamlessly and achieve project objectives.
You may want to implement collaboration tools and platforms to facilitate communication.
Step 7. Implement robust project management software
Invest in project management software that aligns with your organization’s needs.
Such software can assist in project planning, resource allocation, progress tracking, and reporting.
Here is an overview of the top 3 reports available with PM3, BestOutcome’s project management tool .
Step 8. Monitor and evaluate progress
Regularly monitor project progress and evaluate results against predefined objectives.
Use key performance indicators (KPIs) to measure project success and make data-driven decisions.
Adjust strategies and processes based on lessons learned from completed projects.
Step 9. Promote continuous improvement
Encourage a culture of continuous improvement within your organization.
Regularly review project management processes, methodologies, and tools to identify areas for enhancement, while gathering feedback from project teams and stakeholders to refine future project roadmaps.
Step 10. Celebrate successes and learn from failures
Celebrate project successes and acknowledge the efforts of your project teams.
Equally important, learning from project failures or setbacks will facilitate the success of future projects.
Conduct post-project reviews to identify root causes and implement corrective actions to prevent future issues.
Effective healthcare project management requires a unique blend of technical expertise and soft skill sets.
Healthcare projects often involve intricate clinical processes, regulatory compliance, and the coordination of diverse stakeholders, making the role of a healthcare project manager both challenging and crucial.
In this chapter, we explore the essential skills that healthcare project managers need to excel in.
Communication skills
Effective communication is the cornerstone of successful healthcare project management.
Healthcare project managers must convey project goals, updates, challenges, and expectations to a wide range of stakeholders, including healthcare professionals, clinicians, administrators, patients, regulatory bodies, and vendors.
Clear and transparent communication fosters trust and ensures everyone is aligned with project objectives.
Leadership and team management
Healthcare project managers are leaders who inspire and guide their project teams.
Leadership skills are vital for motivating team members, resolving conflicts, and creating a positive work environment within a healthcare facility.
A strong project manager empowers their team to perform at their best, resulting in better project outcomes.
Risk management
The healthcare industry is fraught with risks, from regulatory changes to clinical uncertainties.
Project managers must be adept at identifying potential risks, assessing their impact, and developing strategies for mitigation.
Effective risk management minimizes disruptions and ensures healthcare quality improvement.
Healthcare knowledge
A deep understanding of healthcare systems, regulations, clinical practices, and industry-specific terminology is essential for healthcare project managers in the UK.
They must be well-versed in the NHS structure, public health and health insurance policies, and regional variations to make informed decisions, navigate complex healthcare environments, and bridge the gap between clinical and administrative teams.
Technical proficiency
Proficiency in project management tools and healthcare-specific software is a prerequisite for efficient planning, tracking, and reporting.
Familiarity with Electronic Health Records (EHRs), health information exchange systems, and healthcare analytics tools is valuable for managing healthcare projects effectively.
Regulatory compliance
Healthcare projects in the UK are subject to a myriad of regulations, including data privacy laws (e.g., GDPR), clinical standards (e.g., NHS Digital standards), and industry-specific guidelines.
Project managers must stay updated on these regulations and ensure that projects adhere to them to maintain compliance with NHS requirements.
Change management
Implementing changes within healthcare organizations can be met with resistance from staff or patients.
Healthcare project managers often collaborate with change management experts to facilitate the smooth transition of healthcare teams into new processes, technologies, or workflows.
They must understand change dynamics and how to overcome resistance.
Critical thinking and problem-solving
Healthcare projects often encounter complex challenges and unexpected issues.
Project managers need strong critical thinking skills to analyze problems, identify root causes, and develop effective solutions.
Quick and informed decision-making is critical for project success.
Time and resource management
Project managers must be skilled at resource allocation, time management, and budget control.
Effective resource management ensures that projects stay on track and within budget, ultimately contributing to the organization’s financial health.
Emotional intelligence
Emotional intelligence enables project managers to understand and manage their emotions and the emotions of others.
This interpersonal skill set fosters empathy, effective communication, and better relationships with team members and stakeholders, all of which are crucial in healthcare settings.
Adaptability and flexibility
The healthcare landscape is constantly evolving.
Project managers must be adaptable and flexible, ready to pivot in response to changing circumstances, regulations, or stakeholder needs.
An ability to embrace change and uncertainty is a valuable asset.
Quality assurance
Quality assurance is fundamental in healthcare projects.
Project managers should incorporate quality control measures into projects to ensure that patient care standards are met or improved during and after project implementation.
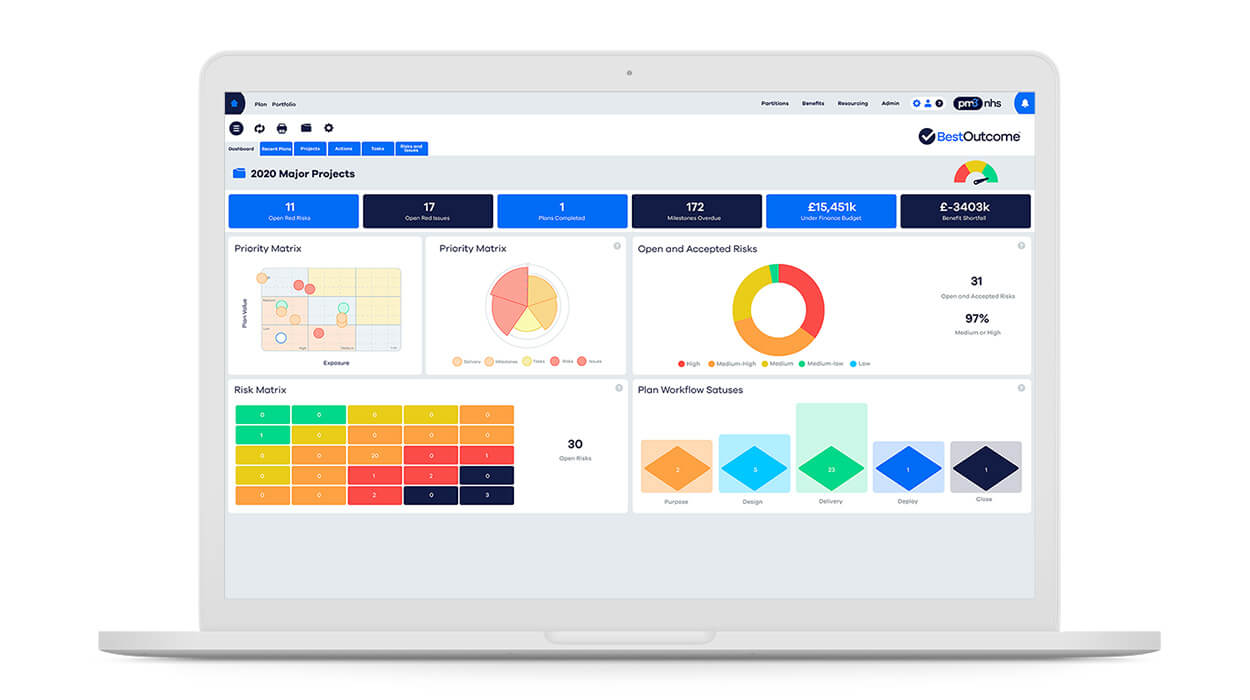
When it comes to project and portfolio management within the National Health Service (NHS) in the UK, one software solution stands out as the preferred choice: PM3.
Developed by BestOutcome, PM3 is the go-to Project, Programme, and Portfolio Management (PPM) tool trusted by NHS organizations for its exceptional capabilities and commitment to achieving successful outcomes.
Why PM3 is the No. 1 NHS PMO Tool
For over a decade, PM3 has solidified its position as the number one NHS PMO tool.
It has garnered a substantial user base that includes a wide spectrum of NHS entities, such as NHS Trusts, Clinical Commissioning Groups (CCGs), Cancer Alliances, Sustainability and Transformational Partnerships (STPs), Integrated Care Systems (ICSs), Integrated Care Providers (ICPs), NHS England and Improvement, Health Education England (HEE), and NHS Professionals.
One of PM3’s distinctive features is its partitioning capability, allowing multiple NHS organizations to operate seamlessly on a single standard instance.
This enables cross-programme collaboration while maintaining data privacy, a crucial consideration within the NHS framework.
Find out more about our NHS success stories.
Outcome-driven functionality for UK healthcare
PM3 sets itself apart as the UK’s sole outcome-driven PPM tool, capable of effectively managing everything from straightforward stand-alone projects to extensive organizational change programmes.
It offers a range of benefits tailored to NHS project managers:
Simplicity for busy NHS Users
Recognizing the demanding schedules of NHS professionals, PM3 has been meticulously designed to be intuitive and user-friendly.
The interface is decluttered, presenting each user with only the screens and information relevant to their specific role.
This streamlined approach greatly reduces complexity, facilitating rapid user adoption throughout NHS organizations.
Tailored configuration for NHS Processes
PM3’s high degree of customization allows you to configure it to align perfectly with your unique NHS processes.
This adaptability ensures that PM3 seamlessly integrates with your specific project and portfolio management needs within the context of NHS healthcare.
Benefits realization
PM3 ensures that your benefit plan is both realistic and attainable, a critical factor in the context of NHS projects where patient care and outcomes are paramount.
Sophisticated reports and dashboards
With over 100 out-of-the-box reports and customizable dashboards, PM3 empowers you to monitor project progress and performance with precision. Furthermore, the intuitive drag-and-drop interface allows you to construct your reports, tailoring them to your NHS organization’s specific needs.
Prioritization and transformation support
PM3 isn’t limited to project management; it is adept at managing programmes and portfolios, facilitating prioritization to ensure that NHS projects receive the necessary focus and resources.
Effective resource management
Understanding resource availability is a central concern for NHS projects. PM3 maintains capacity by role and person, streamlining the resource allocation process. This helps resource managers quickly identify overloaded or underutilized resources, ensuring optimal allocation to safeguard patient care.
Support for agile and waterfall
PM3 accommodates both Agile and Waterfall methodologies, offering features that include user stories, sprints, and kanban boards. This adaptability is invaluable for NHS projects with diverse requirements.
Enhanced team collaboration
PM3 encourages collaboration among dispersed project teams, enabling seamless communication and improved team productivity. Team members can choose to work within PM3 or utilize the PM3Team app, available on Google Play and the App Store.
Partnership with BestOutcome
Selecting PM3 as your NHS PMO tool means entering into a partnership with BestOutcome.
BestOutcome is more than a software provider; it is a team of PPM specialists deeply committed to helping you achieve your project and portfolio management goals within the NHS.
The BestOutcome team offers expert training and mentoring to ensure that you and your team maximize the potential of PM3.
This commitment to your success goes beyond software and encompasses the importance of having trained and enthusiastic users who can leverage the tool effectively
Whether you are managing healthcare transformation initiatives, optimizing patient care processes, or tackling complex healthcare projects, PM3 is the NHS’s preferred choice for clarity amid complexity and delivering tangible results.
For more info about how PM3 can help your healthcare organization, schedule a demo now or contact us at sales@bestoutcome.com

Our products help you deliver successful change programmes and projects by always focusing on the overall business outcomes. Find out how our products can help you.
Are you struggling to understand how to plan a project that keeps you and your team on target? In th...
Read more >